Common Conditions
Heavy periods
Not everyone with heavy periods will want to have treatment. Some patients are happy to be reassured that they don't have a serious underlying problem.
We are able to offer a full range of treatment options for those patients who would like help including the latest day case techniques.
A popular choice at present is a procedure called an endometrial ablation which is a safe and highly effective alternative to hysterectomy for most women. See opposite to play demonstration and below for more details on endometrial ablation.
We hope the following information will help you decide if you are having abnormal periods, the tests which may be necessary to investigate if there is a problem and the different treatment available.
Normal periods
During each menstrual cycle the lining of the womb/uterus thickens and gets ready to accept an embryo if an egg is successfully fertilized. If you don't become pregnant the womb lining breaks down and comes away as a period. A period is the body's natural way to remove the womb lining.
How can it tell if my periods are heavy?
Most women will have a period once a month and bleed for no more than five to seven days. Your periods are probably heavy if:
- You pass clots or have "flooding"
- Double protection is essential (tampons and towels)
- You need to change your tampon more than every two hours
- Blood soaks through your protection into the bed sheets at night
- The period lasts for more than a week
- You have become anaemic
- Your quality of life is being excessively affected by your period
There isn't really an easy or reliable way to measure the amount of blood lost with each period so your doctor will rely on your symptoms (and perhaps a blood test for anaemia +/- iron levels) to decide if your periods are heavy.
What information will my doctor need to know about my periods?
Your doctor will need to ask a number of questions to help diagnose your problem including:
- The length of your menstrual cycle (the number of days between the start of one period and the start of the next)?
- The number of days your period lasts for?
- Do you pass clots or have "flooding?"
- The date your last period began?
- Are you having some bleeding between your periods or after intercourse?
- How painful are your periods?
- Is intercourse uncomfortable?
- Do you suffer from pre-menstrual tension (PMT)?
Why do I need to be examined?
An examination of the abdomen and pelvis is important to try and identify the cause of heavy periods. For example, your doctor may find that the womb is enlarged or there are fibroids, although in the majority of women no obvious problems are detected.
What investigations will be necessary?
a) Blood tests
A blood test to measure your Haemoglobin, and possibly your iron level, will show if you have become anaemic. Sometimes it is necessary to measure hormone levels, particularly if the periods are irregular or there are concerns about the menopause – although this is not always necessary.
b) Ultrasound scan
It may be necessary to arrange an ultrasound scan to check the size/shape of the womb and look at the inner lining (also known as the endometrium). Sometimes a scan will find benign swellings in the muscle wall of the womb which are known as Fibroids - these are a common cause of period problems. The ovaries will also be checked to exclude problems such as cysts.
c) Endometrial Pipelle Sample
Sometimes it is necessary to take a sample of the lining of the womb (endometrium) to make sure that the cells are growing normally. This is called an endometrial pipelle sample. Usually during an outpatient visit a very fine plastic tube is passed through the cervix into the womb and a small specimen is taken which is then checked under the microscope in the laboratory.
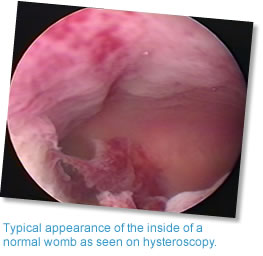
d) Hysteroscopy
This is a procedure which involves passing a small camera though the cervix to look inside the womb to make sure it is healthy. It is most commonly performed under a short general anaesthetic, although some women are suitable to have the operation under local anaesthetic - which means they don't need to be put to sleep. A "D&C" or endometrial pipelle sample is also usually taken to obtain a sample of the lining cells to make sure there is no abnormality. Common problems such as polyps or fibroids can be detected by hysteroscopy and may be removed at the same time.
A hysteroscopy is usually done prior to some treatments such as an endometrial ablation (see below).
What treatment options are available?
Not everyone will require treatment – some patients are happy to be reassured that their periods are normal and no abnormalities can be found either on examination or ultrasound scan. If treatment is required, there are a number of alternatives available.
1. Non hormonal
These tablets can be useful as they are only taken at the time of a period and they don’t have any lasting effects. They can reduce the amount of blood which comes away during a period by up to 50% as well as helping period pains as well.
2. Hormonal
The combined oestrogen/progesterone contraceptive pill or the progesterone only mini-pill are both useful for treating heavy periods and would provide additional contraception. They need to be taken throughout the month.
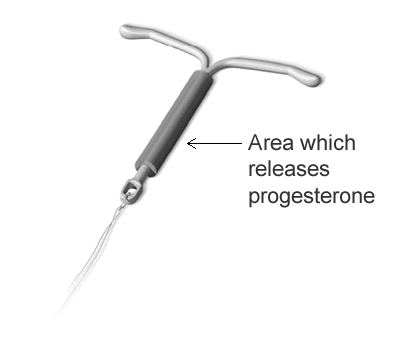
How does a Hormonal IUS help heavy periods?
The Hormonal Intra-Uterine System (IUS) is a contraceptive device which is placed inside the womb. It releases a small amount of progesterone hormone which stops the lining of the womb thickening each month - making periods shorter and lighter.
How does it work as a contraceptive?
The Hormonal IUS makes it difficult for an embryo to implant in the womb. Cervical mucus also becomes thicker which makes it harder for sperm to get into the uterus. Finally, in some cases the Hormonal IUS can temporarily stop the ovaries from producing eggs (ovulating).
How is the Hormonal IUS inserted?
The Hormonal IUS can either be placed in the outpatient clinic or, alternatively, it can be inserted at the time of a hysteroscopy and D&C. The device is passed through the cervix into the womb. The best time to have a Hormonal IUS is either during or at the end of a period when it can be certain you are not pregnant. It is also easier to insert as the cervix is slightly more dilated.
How effective is it for treating heavy periods?
The Hormonal IUS is very effective for most patients with about 70-80% of women finding that it has helped their heavy periods. After approximately three months use, the average blood loss is 85% less and around one third of ladies will stop having periods altogether. This is not a problem because the lining hasn’t thickened up during the month and there is nothing to come away.
How long does the coil last for?
The Hormonal IUS can be left in place for up to five years and then needs to be replaced.
When can I rely on it for contraception?
The coil is effective immediately and no other contraception is required.
How easy is it to remove?
There is a small string at the end of the coil which comes out through the cervix. Removal involves passing a speculum into the vagina and then removing the coil by pulling on the string. There is slight discomfort for one to two seconds.
How much does it cost?
The Hormonal IUS costs around £90-£100. Although this sounds expensive it does, of course, last for five years.
Can it be used if I have fibroids?
The Hormonal IUS can be used if there are only small fibroids within the womb. If there are large fibroids, then this may distort the shape of the uterine (womb) cavity making it difficult to place the Hormonal coil properly.
What happens when the Hormonal IUS is removed?
When the coil is taken out, it is quite likely that you will revert back to your normal bleeding pattern and, of course, your periods may continue to be heavy. Fertility returns very quickly but it is probably best to wait for your next period before trying for a pregnancy so that it is easier to work out how far on you are when you do fall pregnant.
What are the side effects?
1. Irregular periods
It takes approximately two to three months for the Hormonal IUS to work for most ladies. During this time it is very common to have some slightly irregular bleeding which may be on a daily basis initially. The bleeding settles down with time in most patients but unfortunately a few continue to have a persistent, troublesome light period or some discharge.
2. Expulsion
There is an extremely small chance that the coil could come out, particularly if the periods remain heavy. If it is being used for contraception then the coil should be checked after each period to make sure it is still in place. This is done by self examination - if the string can be felt coming out through the cervix then it is still in position. If there is any doubt then an examination should be performed by your doctor or practice nurse.
3. Hormonal problems
The main advantage of the Hormonal IUS over tablets is that the progesterone hormone is delivered directly onto the lining of the womb - only a very small amount gets absorbed into the body. This tends to reduce the risk of hormonal side effects. However, in some ladies this can cause some water retention/bloating. Premenstrual tension (PMT) can also be a concern for a minority of women although this tends to get better with time.
4. Pelvic infection
Although most normal coils increase the risk of pelvic infection, this does not seem to be the case with a Hormonal coil.
5. Contraceptive failure
The Hormonal IUS is an extremely effective form of contraception. If 1000 women used a Hormonal IUS for a year, only one would fall pregnant compared to about ten for the normal coil or 20 for the Pill. As with all coils, if it does fail there is a higher risk of ectopic pregnancy. If you fall pregnant then it is important to see your doctor to rule out an ectopic pregnancy.
The inner lining of the womb is called the endometrium – this is the area which bleeds each month to cause a period. An endometrial ablation is a simple day case treatment which aims to destroy as much of the lining as possible so that less will grow each month, making periods lighter in about 90% of patients.
Several techniques are available but the most commonly used is a Novasure ablation technique. A fan shaped device is inserted into the womb, usually under a short general anaesthetic and some heat is then sent through the lining for approximately 90 seconds.
After slightly dilating your cervix a triangular mesh device is carefully placed inside the uterus (womb) and expands so that it touches as much of the lining (endometrium) as possible.
Precisely measured radio frequency energy is delivered through the mesh for approximately 90 seconds.
The mesh device is removed from the uterus – nothing remains inside the body after the operation.
The endometrium is usually destroyed as shown in this video clip (see below) of the inside of the womb after an ablation.
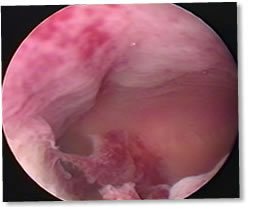 Pre-ablation
Pre-ablation
Post-ablation
An endometrial ablation is a simple and safe alternative to hysterectomy with a short recovery time of normally just a few days. It is not suitable for women with a very large uterus or those who may wish to have further children.
A hysterectomy is an operation to remove the womb. It is the only treatment which is guaranteed to completely stop troublesome periods. For this reason, it is preferred for some patients particularly if they have either tried other options which have been unsuccessful or they have a problem with the womb such as fibroids.
There are several different types of hysterectomy: abdominal, vaginal and laparoscopic ("key hole"). Mr Hextall is trained in all of these techniques.
We hope you will find these Information Leaflets produced by the Royal College of Obstetricians and Gynaecologists (RCOG) useful.
If you would like any further information then please don't hesitate to get in touch.




