Common Conditions
Urinary incontinence

Mr Hextall and his team see at least 20 women each week who are having regular urinary leakage. Our sympathetic and understanding approach aims to put women with this often embarrassing condition at their ease.
A full range of treatment options are available including pelvic floor physiotherapy, medication and surgery – which is most often performed as a day case with a short recovery time.
Many women with incontinence will also have other problems such as prolapse or heavy periods. As Mr Hextall is a Urogynaecologist he can treat both bladder problems and gynaecological problems at the same time.
Urinary incontinence is a really common problem. If this is affecting you please don't feel alone – at least 20% of women will have a problem controlling their urine at some time of their life. There are several types of incontinence:
- Stress incontinence – leakage with coughing, sneezing or exercise
- Urge incontinence – women develop a sudden urge to reach the toilet and often start leaking before they make it.
- Mixed incontinence – patients have a mixture of stress and urge leaks
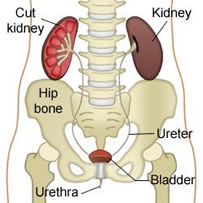
This is the most common cause of urinary incontinence in women and is often caused by a weakness of the ligaments or muscles under the bladder. There are 2 main treatment options:
Pelvic floor physiotherapy
Pelvic floor exercises / physiotherapy can improve the bladder control of approximately 60% of women with stress incontinence – it is therefore usually a good idea to try this before considering surgery as an operation may not be necessary. The exercises can work very quickly for some women who regain "The Knack" of squeezing their muscles at the correct time. Sometimes it can take several weeks to fully regain the strength in the muscles around the bladder.
Physiotherapy also involves advice regarding your own anatomy (and what has gone wrong), lifestyle changes, bladder retraining and fluid modification. Pelvic floor stimulators or vaginal cones (see image below) can also be used.
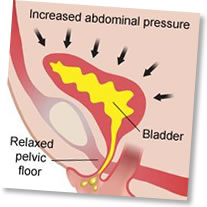
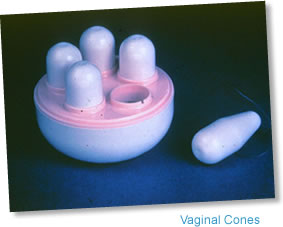
Pelvic floor exercises can be taught by Jackie Walker (Urogynaecology nurse specialist Jackie Walker). In addition we work closely with the physiotherapy teams at Spire Hospital Harpenden, Spire Hosiptal Bushey and the Redbourn Physiotherapy clinic.
Surgery
Section currently under redevelopment.
There are a number of causes of urge incontinence and sometimes it is necessary to perform some tests to see what is happening.
Many women have urgency because they have an Overactive bladder. This condition has a number of other names including detrusor overactivity, detrusor instability, irritable bladder and unstable bladder.
An overactive bladder squeezes when you don't want it too. It is often a worse problem than stress incontinence because urgency may come on suddenly and a large volume of urine can leak – causing urge incontinence. Often women have other troublesome symptoms such as urinary frequency and they make have to get up several times each night - disturbing their sleep.
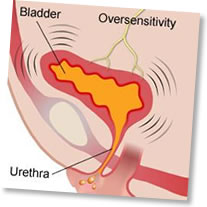
What causes an Overactive bladder?
No one is sure why an overactive bladder develops. Some patients remember having problems controlling their urine as a child – perhaps they were a late bed wetter, frequently had to leave the class to pass urine while at school or had accidents in the playground while laughing with friends. Other women develop symptoms of urgency as they get older and may find they have to rush to pass urine if they listen to running water, wash their hands or put the key in the door. There are lots of theories why an overactive bladder may develop. It may be that the bladder muscle becomes irritable, the nerves to the bladder are oversensitive or the area in the brain which controls the bladder is malfunctioning.
What treatments are available?
1. Fluid modification. Sometimes patients drink a lot of tea, coffee or caffeinated drinks which may irritate the bladder and make the symptoms of frequency or urgency worse. It is often useful to complete a bladder diary so that we can accurately record how much fluid is taken in during the day, the number of times a patient goes to the toilet and the amount passed each time. Using this information, some women are asked to drink a little more (if they are not drinking enough then the urine can become very concentrated and this may irritate the bladder) or, alternatively, reduce their fluid intake because if they are drinking too much, this may make them go to the toilet even more often.
2. Bladder retraining. Many patients have got into the habit of doing to the toilet "just in case" because they are worried about developing urgency and leaking. Over time this means that the bladder will hold less and less so making the symptoms of an overactive bladder worse. Bladder retraining is used to try and gradually increase the time between visits to the toilet so that eventually the bladder holds more urine and patients gain greater control. Further information on bladder retraining can be found here.
3. Physiotherapy. Many patients find that pelvic floor exercises, often under the supervision of a physiotherapist, can improve bladder control. As well as strengthening muscles, the physiotherapist will teach some distraction techniques, (e.g.) thinking of work or holiday while you have a strong desire to go to the toilet can make this sensation disappear over 30 seconds or so, and then you can calmly walk to the lavatory.
4. Medication. Many tablets are available to try and calm the bladder and stop it squeezing when it shouldn't. A patch can also now be used. Approximately 60-70% of patients will gain some improvement with the medication. Unfortunately, it has to be used long term and some patients can develop side effects such as dry mouth or constipation.
5. Posterior Tibial Nerve Stimulation (PTNS) is a new treatment for urinary frequency and urgency, most commonly caused by an overactive bladder. It is now available under Mr Hextall's care at St Albans City Hospital (NHS) and is undertaken by one of the 3 excellent Urogynaecology nurse specialists working there.

PTNS is a form of neuromodulation which can be used with, or as an alternative to, other treatments such as fluid modification, bladder retraining and anticholinergic medication.
The treatment targets the tibial nerve in the ankle and modifies the nerve impulses sent to the bladder which contribute to the development of urgency. A small acupuncture needle is inserted into the ankle near the Tibial nerve and is then connected to a stimulator device.
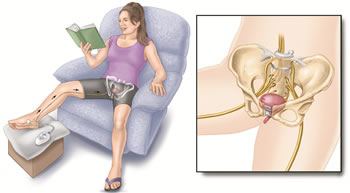
At the end of twelve 30 minute outpatient sessions, usually undertaken once or perhaps twice per week, there is a 70-80% chance of improvement. Sometimes further "top ups" are given depending upon the initial response. Patients have some slight tingling when the needle is inserted but then do not feel anything while the treatment is taking place.
Side effects are minimal and so far the treatment has been very well tolerated.
Are there people who should not use Urgent PC?
- Patients with pacemakers or implantable defibrillators
- Patients prone to excessive bleeding
- Patients who are pregnant or planning to become pregnant during the duration of the treatment
PTNS has recently been approved by NICE and is now one of range of therapies Mr Hextall offers at St Albans City Hospital (NHS) for urinary urgency and urinary incontinence.
Please click here for further information.
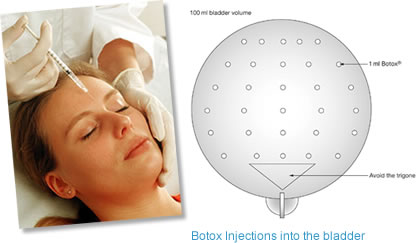
6. Bladder Botulinum injections. Botulinum toxin has been used for cosmetic reasons for many years and it is now licenced to treat bladder overactivity, which is one of the most common causes of troublesome symptoms of urgency, frequency and urinary incontinence. Click here for Bladder Botulinum information sheet.
7. Surgery. Women with Mixed Incontinence (an overactive bladder and a weakness causing stress incontinence) may benefit from surgery but usually only when the bladder has been calmed down by medication.
Sometimes it is possible to determine why someone is leaking based on their symptoms and an examination. However, it may be necessary to perform some tests to gain more information which will show which treatments will be required. These include:
- A urine sample – to exclude infection, diabetes and blood in the urine
- A bladder diary – information regarding how many times a patient passes urine and the amount they drink can be really useful. If possible it helps to complete a bladder diary for a couple of days and then bring this to your first appointment. Click here for Bladder Diary information sheet.
- Urodynamics – It is not necessary to perform this test in all patients but urodynamic studies do provide lots of information about why someone is leaking, and may detect the cause of other symptoms such as urgency or difficulty emptying. Click here for Urodynamic Studies information sheet.
If you would like any further information then please don't hesitate to get in touch.




